
The first round of claims data under the new Medicare payment model for nursing homes shows that the majority of operators are seeing reimbursement boosts — while some are also making key billing mistakes that could result in missed payments for certain services.
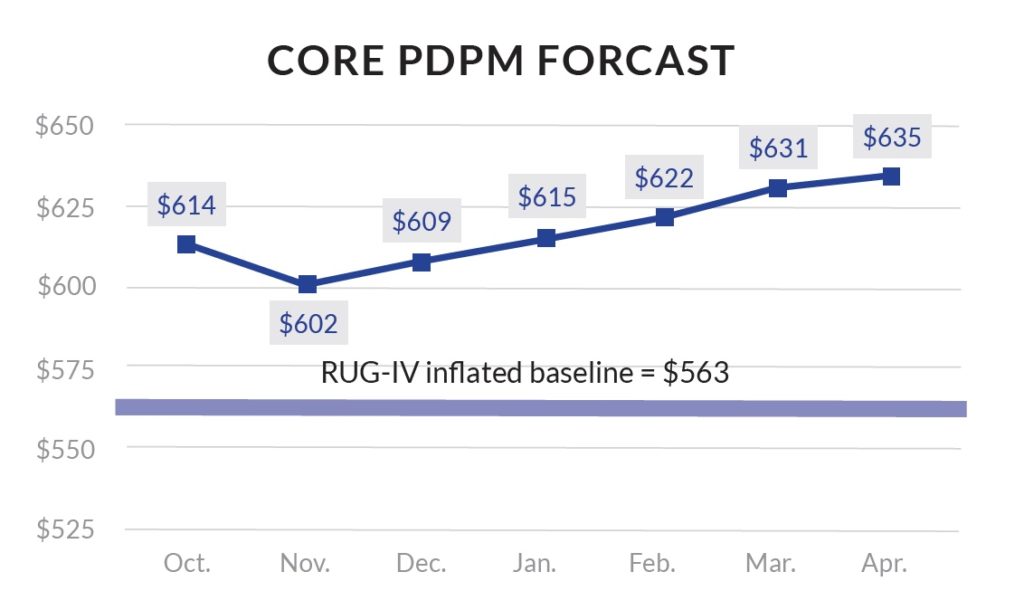
The average skilled nursing facility saw Medicare reimbursements of $614.96 per patient day in October, the first month of the new Patient-Driven Payment Model, according to an analysis from Zimmet Healthcare Services Group and its affiliated data service, CORE Analytics.
For comparison, the average figure under the old Resource Utilization Group (RUG) system was $562.89, for a gain of about $52 per day.
Of the 623 SNFs included in the consulting firm’s analysis, 91.5% saw some kind of increase under PDPM, while just 8.5% — or 50 buildings — had their reimbursements slip.
Those numbers are inflated due to the way that the Centers for Medicare & Medicaid Services (CMS) handled the transition to PDPM; residents already staying at a nursing home on October 1 were considered new admissions, giving facilities a rate boost that won’t be replicated moving forward, Zimmet observed in its report.
But even adjusting for that factor, the average PDPM rate came in at $584 per day, according to the firm’s analysis, or an overall gain of $26.
“Financially, October 2019 claims support our belief that PDPM will not maintain budget neutrality, making a rate recalibration (reduction) likely at some point,” the company warned.
That trend will only continue moving forward, Zimmet projected, with the average daily rate climbing to $635 by April.
This could eventually prove to be a problem for both operators and the federal government, as PDPM was explicitly designed to be revenue-neutral — that is, aside from a routine 2.4% market-basket increase to Medicare rates, CMS plans to spend no more or less money on skilled nursing care under PDPM than it did before.
Most operators and investors echoed this sentiment in the lead-up to PDPM’s implementation, predicting that they’d come out ahead largely on expense reductions related to more efficient therapy programs.
“If this proves even close to accurate, CMS may need a bigger budget,” the firm noted.
The Morganville, N.J.-based reimbursement consulting firm collected more than 20,000 claims from a roster of 623 SNFs within its CORE database, representing operators in 35 states and the District of Columbia as of November 17.
Despite the overall upward trend, curious patterns have already started to emerge on an individual building level, particularly around accurately recording resident conditions — a central tenet under PDPM, a system that brings newfound reimbursement potential to services that operators have always provided.
For instance, in the speech-language pathology (SLP) category, the Zimmet team found that a significant number of patients were listed as having an acute neurological diagnosis, cognitive impairment, and an SLP-related comorbidity, but not a swallowing disorder or a mechanically altered diet. That particular collection of diagnoses is something that Zimmet Healthcare Services Group president Marc Zimmet described as an example of an “impossible combination.”
“Can you imagine someone having acute neurologic, speech disorder, and cognition, and no mechanically altered diet or swallowing disorder?” he told SNN. “Or 60% not having cognition — it’s really amazing when you take a broad look at it, and think about what it means that we’re representing.”
Another area where operators seem to be missing out: depression, a diagnosis that Zimmet chief innovation officer Steven Littlehale described as a “linchpin to PDPM success” in a presentation earlier this year due to its positive effects on both the bottom line and overall resident outcomes.
“If you take anything from this report, please review your October billing and count how many of your Nursing scores end in 2,” the company noted in its report. “If you don’t find any, your facility is either incredibly pleasant and soothing, or you’re leaving upwards of $35 Medicare/day on the table; our advice is to pick them up.”
Though Zimmet and CORE didn’t release state-level data, Marc Zimmet noted to SNN that states with Medicaid systems based on case mix tended to perform better at capturing diagnoses such as depression, with a vast gulf even between the neighboring states of New York — a case-mix state — and New Jersey, which doesn’t use the system.
“It’s just so different than it was under RUGs,” he said. “And as much as I’ve thought about it over the last year and a half, this really was an educational exercise for me — a new way of thinking.”
Moving forward, Zimmet advised skilled nursing staffers to think carefully about the claims they submit, focusing on the story that the numbers and different diagnoses tell — and specifically making sure that story makes sense.
“We invested in that restorative nursing program, but we’re only capturing 5% of the patients in restorative nursing,” Zimmet said, providing an example of a story that doesn’t quite fit. “It’s critical thinking, to put all the pieces together.”
Editor’s Note: Zimmet Healthcare Services Group sponsored an e-mail distribution of its October PDPM report to Skilled Nursing News readers, but the sponsorship had no bearing on SNN’s editorial coverage of its contents or conclusions.



