Therapist staffing coverage at nursing homes fell up to 10% after the October 2019 implementation of a new Medicare payment model, a new study has determined — with the cuts coming primarily on the backs of contracted employees and not full-time skilled nursing facility staffers.
Physical and occupational therapist staffing was 6% lower in the fourth quarter of 2019 than over the same span in the previous two years, while therapy assistant levels in both disciplines were down 10%, according to a study published Monday in the journal Health Affairs.
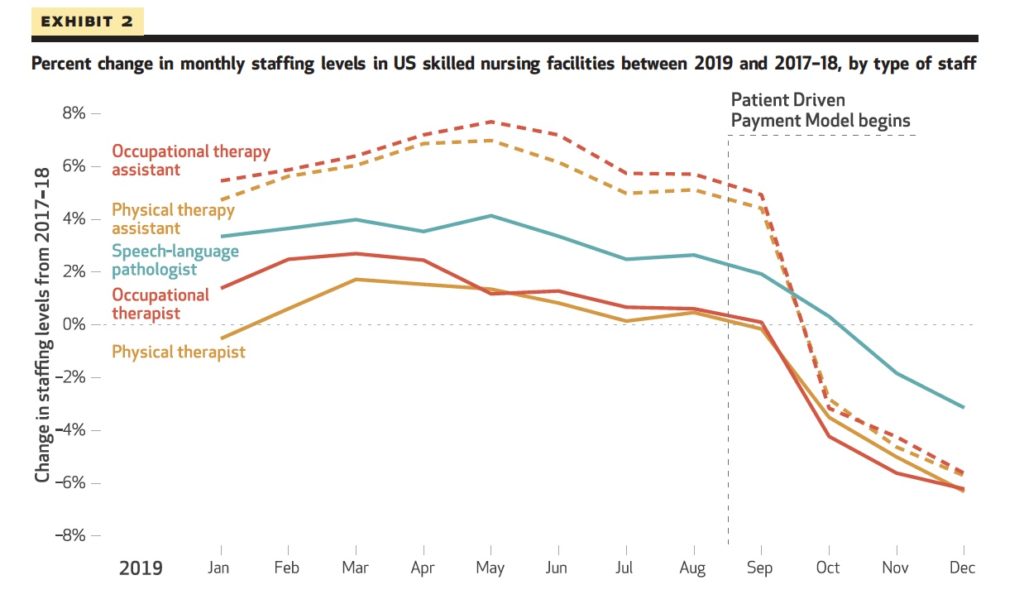
The study marks the first academic probe of care patterns after the implementation of the Patient-Driven Payment Model (PDPM) for post-acute Medicare coverage at the start of the federal government’s fiscal 2020.
Anecdotal reports of therapy cutbacks were widespread that fall as operators looked to adapt to the new model, which more closely links nursing home payments to resident conditions — while also eliminating the financial incentive to provide as many therapy minutes as possible.
Genesis HealthCare (NYSE: GEN), for instance, laid off 5% of its therapy staff as PDPM took effect in October 2019, and trade groups for professional therapists raised concerns about both member employment and resident outcomes under the new system.
The Centers for Medicare & Medicaid Services (CMS) specifically pointed to the potential for fraud reduction as a key feature of PDPM, though both therapy providers and resident advocates sounded alarms about the pendulum to swinging too far in the other direction; while the financial incentive to provide unnecessary therapy services disappeared essentially overnight, the new model introduced the potential for providers to cut back on necessary services in order to save money.
“We didn’t ask this question, but a significant number of members reported layoffs or decreased hours or services,” Sharmila Sandhu, vice president of regulatory affairs for the American Occupational Therapy Association (AOTA), told SNN in February 2020.
The COVID-19 pandemic scrambled the ongoing analysis of PDPM, with the industry focused far more on managing a deadly disaster than fine-tuning a rehabilitation payment model. Group and concurrent services — which observers had expected to increase significantly as therapy changed from a revenue driver to a cost center — became impossible amid federal and state bans on communal activities, and sharp declines in post-acute admissions to nursing homes emerged as the much bigger financial and operational trend of 2020.
But the fourth quarter of 2019, the first three months of PDPM and the last full quarter of pre-COVID normalcy, did reveal some concrete patterns, most of them at the expense of third-party therapy staffers.
“Contract staffing accounted for all of the overall effect for physical therapists, 92% of the effect for physical therapist assistants, 100% for occupational therapists, 93% for occupational therapy assistants, and 133% for speech-language pathologists,” the researchers concluded.
These non-facility workers offer nursing home administrators more flexibility over staffing levels, the team observed, making them easier targets for cuts amid a payment sea change.
“As SNF administrators prepared for the PDPM, it is likely that many made decisions regarding their use of in-house therapists versus third-party therapy companies based on assumptions of how their revenue streams would be affected under the PDPM,” they wrote. “It will be necessary to follow these trends over time to see whether the lower use of contract staff continues as SNFs recalibrate their business models in response to the PDPM.”
The steeper cuts observed among assistants had a two-pronged explanation, according to the researchers, stemming from both a temporary pre-COVID bump in group and concurrent services and a lower frequency of required assessments under the new model.
“Although both therapists and therapy assistants can treat patients, only therapists are licensed to complete assessments,” the researchers wrote. “Fewer required assessments may allow therapists more time to treat patients, thereby reducing demand for therapy assistants.”
The study authors acknowledged that the timing of COVID-19 clouds any analysis of PDPM, while also identifying resident outcomes as a primary question for further research.
“It is unclear, however, whether reductions represent a ‘right-sizing’ of therapy departments that were previously designed to deliver financially motivated therapy of limited clinical benefit, or a form of skimping that limits patients’ access to needed rehabilitation services,” the team wrote.
The study was conducted by Brian McGarry of the University of Rochester; Elizabeth White, Linda Resnik, and Momotazur Rahman of the Brown University School of Public Health; and David Grabowski of Harvard Medical School. The analysis drew on CMS staffing data from 14,525 skilled nursing facilities across the country.


