Occupancy at the nation’s nursing homes cratered during the COVID-19 pandemic, as hospitals suspended non-emergency surgeries and families looked to avoid institutional care settings for their loved ones at all costs.
During the initial coronavirus wave last spring, leaders in the sector hoped that the second half of 2020 would bring a return to normalcy and a reversal of both trends; with heads in beds representing the primary income stream for any given nursing facility, an uptick in referrals is the fastest way for the sector to return to some kind of financial normal after the worst year in its history.
But as 2021 dawned, the coronavirus still raged out of control across the country and nursing home census figures sat at historic lows, and an analysis of post-acute referral patterns shows little sign of significant positive shifts.
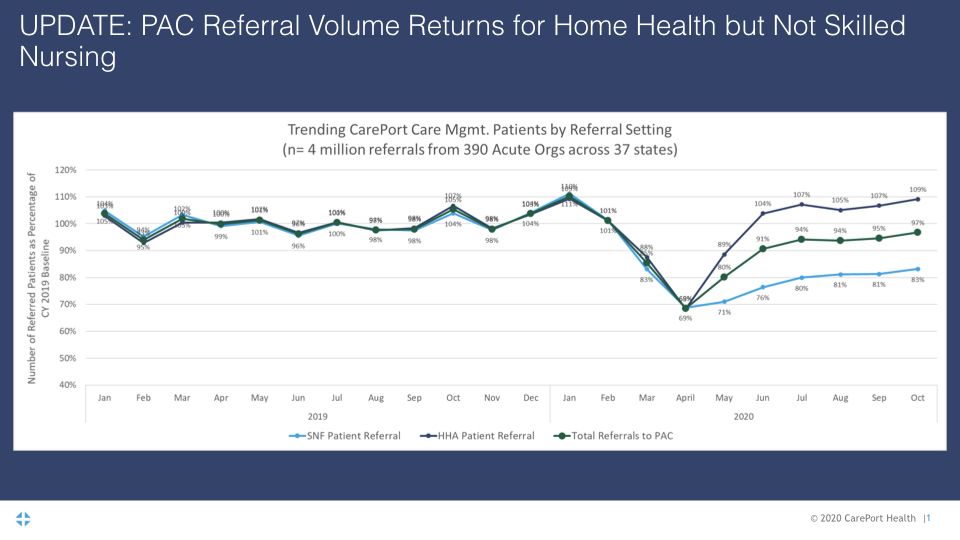
After falling to 69% of the previous year’s volume in April 2020, referrals to all post-acute care settings returned to 97% by October, according to an analysis from care coordination software provider CarePort.
The Boston-based firm drew on its database of discharge information from 390 acute-care organizations across 37 states to track the trends over the course of 2020.
As soon as June, home health agencies were running above their previous capacity, with referrals to the setting reaching 109% of 2019 totals by October. At the same time, skilled nursing facility discharges had only crept back to 83% of historic volume.
“I won’t venture a guess on what that percentage is going to be, but I do not think we’re going to go back to 2019 normal completely,” CarePort director of post-acute analytics Tom Martin told SNN earlier this month.
The analysis validates a growing narrative within both the skilled nursing and home health industries, according to Martin.
“It looks like it’s plateaued, and I suspect we’re going to continue, over the next few months, to see that creep up,” he said. “But we’re still down 15% to 20% from what we saw in 2019 — and so it’s probably not surprising to anyone, but we are seeing that a lot of these patients that have typically gone to skilled nursing are now going to home health.”
As early as last summer, leaders in the home health space touted their census strength relative to their institutional counterparts during the coronavirus crisis. At home health and hospice giant Encompass Health Corporation (NYSE: EHC), for instance, Medicare referrals had returned to 98% of normal by July while skilled nursing census had not recovered.
“All of that would lead us to believe that we’re getting some SNF patients that we wouldn’t have otherwise gotten, particularly directly from physicians,” April Anthony, CEO of Encompass’s home health and hospice business, said at the time.
Paul Kusserow, CEO of fellow home health and hospice giant Amedisys Inc. (Nasdaq: AMED), in particular focused on the 10% to 15% of patients who could go either to home health or a SNF — a cohort he described as “jump-ball business.”
“We have not seen a material recovery in elective procedures, yet we have seen a significant recovery in our admissions, which means we are winning market share and new referral sources,” Kusserow said in July. “Our admissions would also suggest that we are starting to realize the trend of patients wanting to avoid admission into SNFs and other facility-based settings. It is without a doubt that the home is the safest place to care for patients.”
Encompass even identified its inpatient rehabilitation facilities — a more intensive post-acute care niche — as potential competition for SNFs moving forward.
“From a post-acute perspective, the patients that we’re treating in our IRFs really cannot go directly home from the hospital,” Encompass CEO Mark Tarr said last summer. “They require an inpatient stay. So those patients, it becomes a choice between an IRF and SNF in almost all cases — and I would ask you for your opinion as to how the skilled nursing facilities have distinguished themselves during this pandemic.”
The occupancy picture for nursing facilities has not improved since then. The new year began with census of 80% or lower in all of the lower 48 states, according to a recent analysis from professional services firm CliftonLarsonAllen — with figures as low as 56% in Texas.
“Given historically low margins, post-COVID occupancy at even 90-95% of pre-COVID levels will push most operators into a negative margin situation,” CLA principal and senior living segment leader Stephen Taylor and director Seth Wilson observed.
CarePort’s Martin admitted that he doesn’t have a crystal ball for the future, and suggested that the vaccine rollout could be a “game-changer” for traditional institutional nursing home care. But he was also blunt about the prospects of a bounce back to pre-pandemic highs.
“I would not be surprised [if] certainly some portion of these patients, these types of patients that have gone to home health — I think they will continue to do that, and that these percentages are not going to go back to what we saw in 2019,” Martin said.
The perception of slow progress on the vaccine rollout continues to generate negative headlines for the space, and in part prompted at least one financial firm to downgrade a pair of real estate investment trusts (REITs) with substantial skilled nursing holdings.
“While we continue to believe the U.S. government will support the sector through the COVID-19 pandemic, we are entering a new administration and it is somewhat unclear if future stimulus packages will provide additional funding as robust as the CARES Act,” Mizuho Securities USA observed earlier this month, prior to the inauguration of President Biden. “A slow vaccine roll-out in the U.S is also likely to delay the recovery of the skilled nursing segment.”
And for both families and hospital referral leaders, the perception of safety is just as important as the actual progress.
“We’ve seen a lot of — and unfortunately, sometimes, I don’t think fair — media coverage of the skilled nursing industry, and I think that might scare some people off,” Martin said. “Of course, consumers are going to want to receive care at home if the home health agency can do that safely, and it certainly seems like they’re making efforts to do that.”
Those efforts have included more aggressive “SNF-at-home” programs, which seek to increase the acuity that home health agencies can handle; Amedisys as early as last summer was boosting its investments in telemedicine and dialysis to achieve that goal.
“If it can be done in the right way, you can see a complete shift of the type of patients that normally will spend weeks in the SNF before they go home; [they] can actually go home and get that same care in the home,” Amedisys chief operating officer Chris Gerard said at the time.
Sheer admission volume isn’t the only number that will be important to watch over the coming year, however. The Centers for Medicare & Medicaid Services (CMS) may have frozen quality measures for nursing homes given the disparate effects of the pandemic, but that reporting is slowly coming back — and it could have a further impact on the decisions that hospitals and families make.
“Different providers have gotten hit with the pandemic at different times,” Martin said. “Sometimes the best providers are taking your COVID patients, and it really messes up their quality measures. So they might look worse, even though they might be one of the better in your market.”
Companies featured in this article:
Amedisys, CarePort Health, Centers for Medicare & Medicaid Services, CLA, Encompass Health, Mizuho Securities USA



