When elective surgeries were halted or suspended in spring in an attempt to preserve hospital capacity, the number of patients leaving the hospital setting dropped significantly — and the number of patients leaving that setting for skilled nursing fell by nearly half as well.
A new analysis of all Medicare fee-for-service claims data from January through May, and paid through June, from consulting firm ATI Advisory highlights the effect of the pandemic on both hospitals and SNFs.
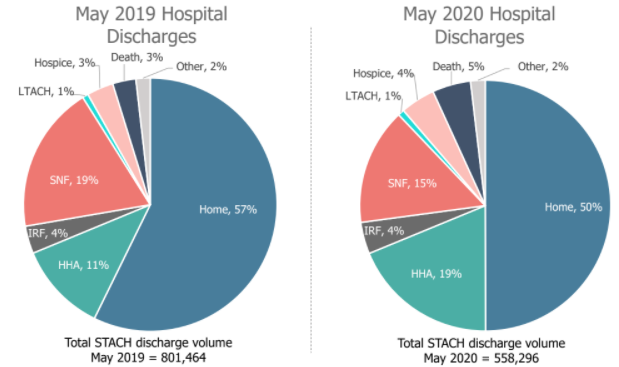
In May 2019, the total discharge volume from short-term acute care hospitals was 801,464, according to the claims data. Of that total, SNFs received 19%.
In May 2020, the total discharge volume came in at 558,296 — and SNFs received 15% of that.
“When we think about the impact on skilled nursing facilities, they’re getting a double whammy,” ATI Advisory CEO Anne Tumlinson told Skilled Nursing News in a November 18 interview. “The double whammy is that the size of the available referrals has dropped … so they’re getting a smaller share of a smaller pie. That’s why it feels so dramatic to them. Meanwhile home health and to a certain extent, hospice … are getting a larger share of the pie.”
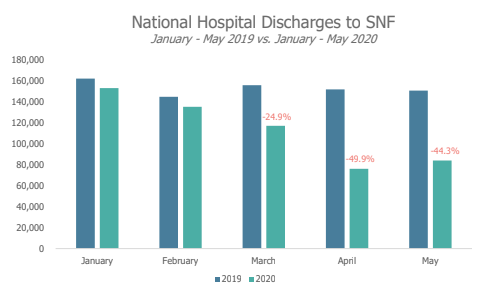
In April, the decline in hospital discharges to the SNF setting was even more dramatic, as Elizabeth Burke, an analyst at ATI who designed and conducted the update on the claims data, pointed out.
Specifically, hospital discharges to SNF nationally fell 49.9% from April 2019 to April 2020. From May 2019 to May 2020, they fell 44.3%.
The time lag for the Medicare fee-for-service claims data means that the numbers give a good encapsulation of the impact of the COVID-19 pandemic during the spring, but it is a snapshot of a fairly specific time period, both Burke and Tumlinson noted.
Still, the data appear to bear out forecasts in the pandemic’s early days that predicted major challenges for SNFs stemming from the suspension of elective surgeries.
Another study from the consulting firm Avalere Health in September found similar results on the number of hospital discharges sent to the SNF setting.
But SNFs came out ahead for one particular cohort of hospital discharges: those with a COVID-19 diagnosis code, the ATI Advisory study also found.
Tumlinson noted that this does not mean that the patients sent to a SNF from a hospital were necessarily positive at the time of discharge; they may have been hospitalized and only gone to the SNF setting after they became negative for the virus.
But regardless of positivity at discharge, SNFs received the highest share of discharges of COVID-19 diagnoses among post-acute care settings, the ATI study found. Specifically, SNFs received 25% of a total of 104,886 COVID-19 hospital discharges from January through May of this year.
There is one additional component of the COVID-19 discharges that could explain why SNFs received more of them, Tumlinson said: Long-term care residents were the ones who were most affected by COVID-19 in March, April, and May.
“They probably were hospitalized briefly, and then they’re going to come back into the SNF where they lived as a short-term post-acute care patient,” she said.
ATI Advisory wants to do some additional examination of the geographic breakdown of COVID-19 discharges to SNFs, Tumlinson said, given pushes by states such as California and New York to free up hospital capacity by sending patients to the SNF setting. And Burke noted that especially in the early months of the pandemic, some patients might have had COVID-19 without getting that diagnosis, possibly being designated as the flu.
Burke would want to examine patient characteristics in future studies, as well as how many hospitalizations some of the COVID-19 patients experienced.
“We’re definitely really interested to see how these trends that we’re seeing here either continue, or just completely changed course in the later months of the pandemic,” Burke said.


