News of therapy layoffs swept through the skilled nursing industry in the weeks after the implementation of the Patient-Driven Payment Model (PDPM), and a new poll from Skilled Nursing News finds that more than 40% of operators and therapy vendors have made some kind of staffing reductions post-October 1.
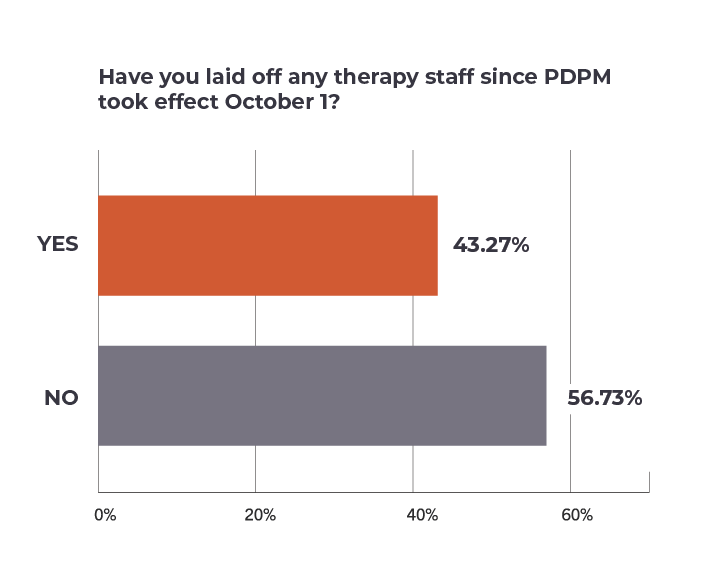
A little more than 43% of respondents reported that their firms laid off therapists in the immediate wake of the new Medicare payment model, compared to nearly 57% that did not change their staffing levels.
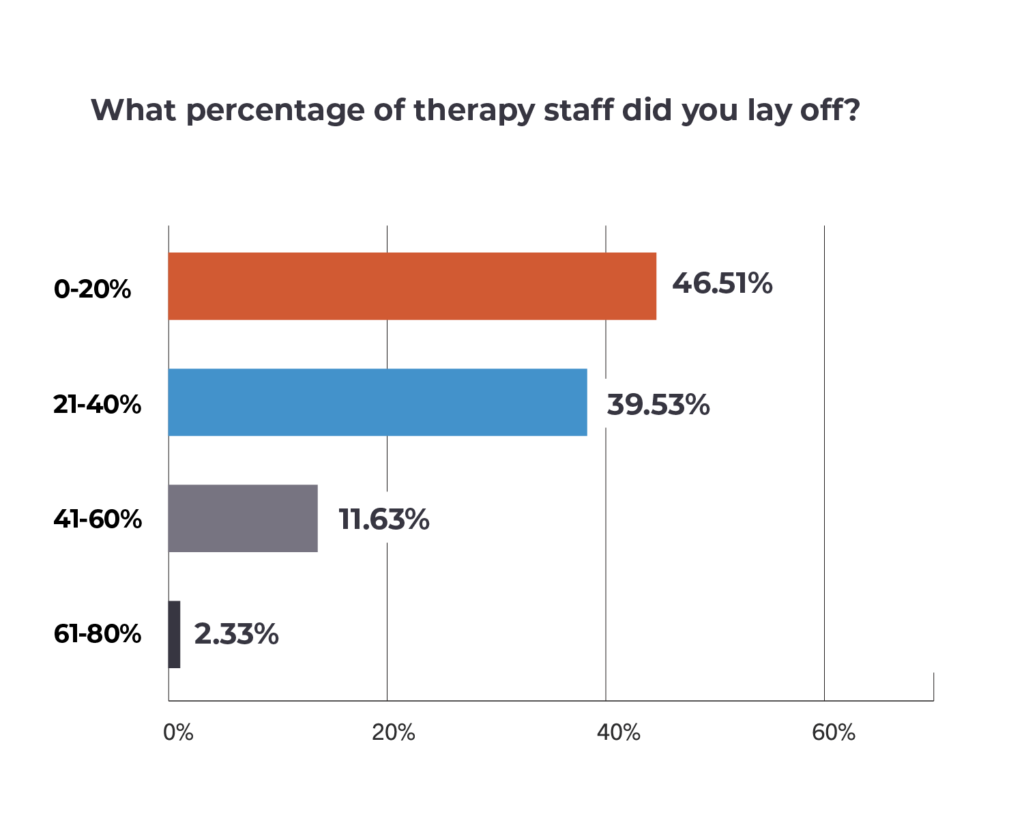
Among those providers and therapy vendors that reduced staff, a plurality — 46.5% — reported that layoffs affected 20% of their workforce or less, with an additional 39.5% instituting headcount cuts of between 21% to 40%.
Reductions in therapist positions have been one of the immediate byproducts of the new reimbursement system, which the Centers for Medicare & Medicaid Services (CMS) explicitly designed as a way to combat potentially unnecessary therapy interventions. By linking Medicare payments more closely with resident acuity — instead of just the volume of minutes — the federal government intends for residents to receive more individually tailored care with a lower possibility of profit-driven therapy provision.
The question of whether providers had been artificially boosting therapy minutes to cash in on Medicare reimbursements had plagued the industry for some time, with stories in the New York Times and Wall Street Journal probing the potential connection between financial considerations and inappropriate care plans. (For its part, the Times this past week published a piece that raised concerns over the opposite effect — patients not receiving enough therapy now that minutes no longer equal dollars — happening under PDPM.)
Whatever CMS and the industry expected in the lead-up to the new model, news of layoffs came swiftly after PDPM’s October 1 implementation: Industry giant Genesis HealthCare (NYSE: GEN) cut its therapy staff by 585 jobs, or about 6% of its overall therapist workforce, right from the start of PDPM, while anecdotal reports of job losses and hour cuts continue to flow into SNN’s inboxes from therapists across the country.
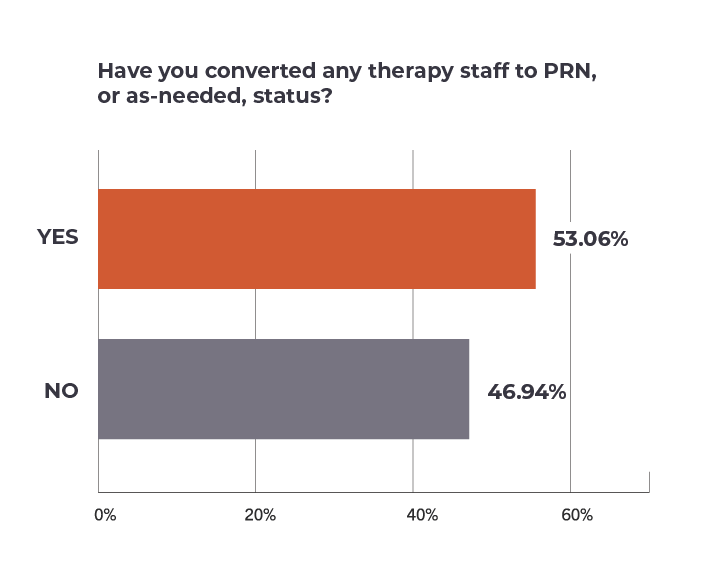
Simply reducing headcount is just one lever that providers can pull to adapt to the new system. More than half of respondents, or about 53%, said they had switched some therapy staff to PRN status, a term that refers to as-needed labor as opposed to steady hours.
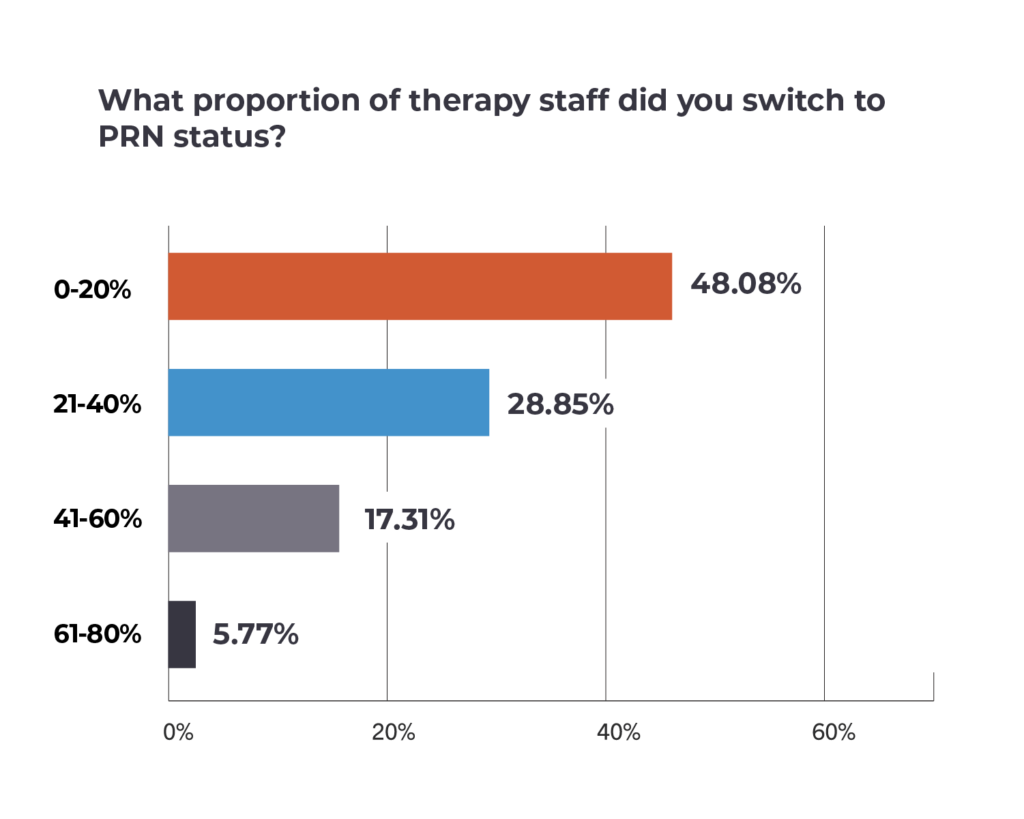
As with layoffs, the PRN shifts were concentrated in the 20% or less range, with only 17% of respondents saying that they had moved between 41% and 60% of workers to the status — and just under 6% converting between 61% and 80% to PRN.
Finally, SNN asked respondents about their use of group and concurrent therapy — modalities that many operators have touted as a way to both reduce costs and improve resident outcomes, primarily through the purported social benefits of conducting therapy with peers. Genesis, for example, estimates that the combination of group-therapy boosts and headcount cuts will save the company $30 million per year going forward.
“We did some research studies and found that appropriate use of group and concurrent therapy can actually be at least equal — if not better, or more efficacious — than one-on-one therapy in certain cases,” Genesis CEO George Hager said last month.
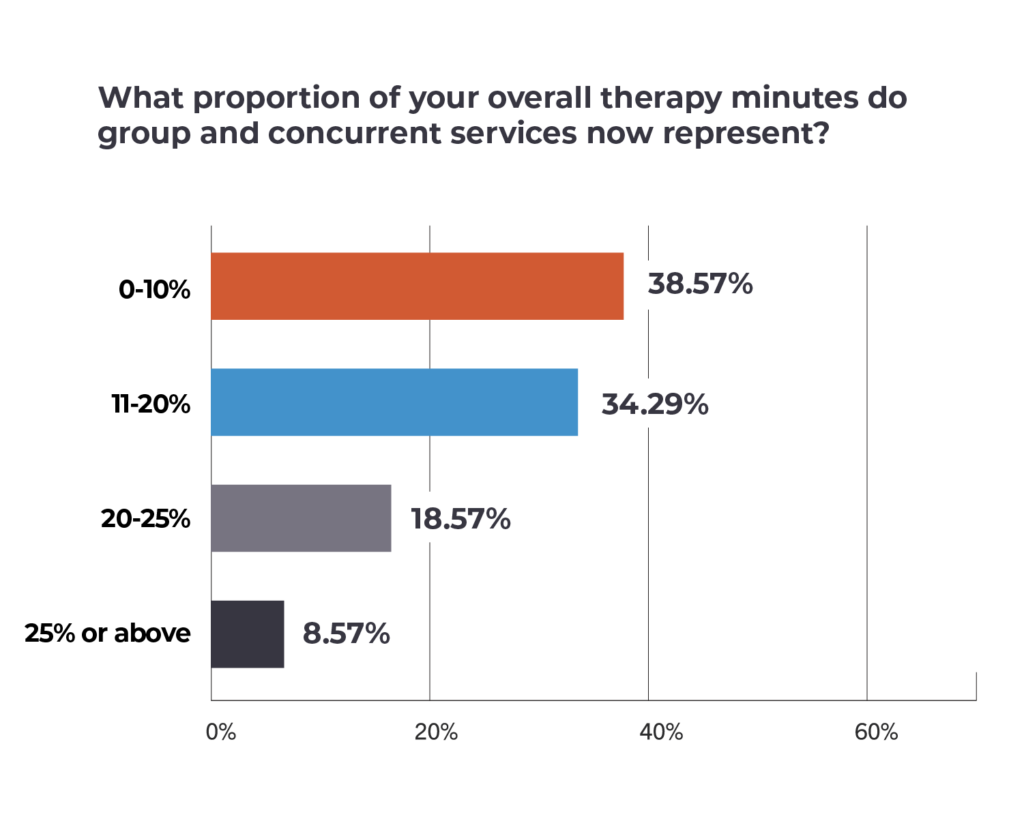
A full 75% of respondents told SNN that their companies had increased the use of such services since October 1, which under the new model cannot account for more than 25% of each resident’s overall therapy plan. So far, at least according to SNN readers, the exact proportions seem to be settling within the up-to-20% range.
SNN limited the poll, conducted via voluntary responses to a set of questions hosted on SurveyMonkey and promoted several times on our website and in our morning newsletters, to operators of nursing homes and third-party therapy providers. The poll was open from October 29 to November 24.
In all, we collected responses from 111 users who self-identified as operators, though individual questions had lower engagement — ranging from 104 to 24 respondents. SNN acknowledges that the poll was not scientific; we instead intend to provide a snapshot of early sentiment and strategy at a critical time in the skilled nursing industry.
We welcome all reactions to the poll and its results; please contact editor Alex Spanko at [email protected] to weigh in with your opinions, constructive criticisms, and general comments.



