Massachusetts has been at the forefront of nursing home stress over the last few years, and a new government report illustrated a host of negative statistics — from cratering utilization to median margins as low as -10% for the worst-performing properties.
In terms of total resident days, nursing facility utilization in Massachusetts dropped 5.4% between 2013 and 2017, or a decline from 15.1 million to 14.3 million.
That’s one of the many conclusions in a November report from the state’s Center for Health Information and Analysis (CHIA), an independent government agency that probes health care trends in the Bay State.
Perhaps unsurprisingly, a decline in Medicare days primarily drove the falling utilization numbers, with a 14.8% drop between 2013 and 2017 — as compared to a 3.4% slide for Medicaid and a 4.8% decrease in self-pay days.
“Nationally, research has suggested that declining utilization of skilled nursing facilities among traditional Medicare beneficiaries may be due, in part, to fewer hospital inpatient discharges among this population, reducing the need for post-acute care,” the Boston-based CHIA concluded. “These trends reflect a number of factors, including Medicare policy initiatives aimed at reducing unnecessary and avoidable hospitalizations, such as promoting accountable care organizations, bundled payment arrangements, and readmissions penalties.”
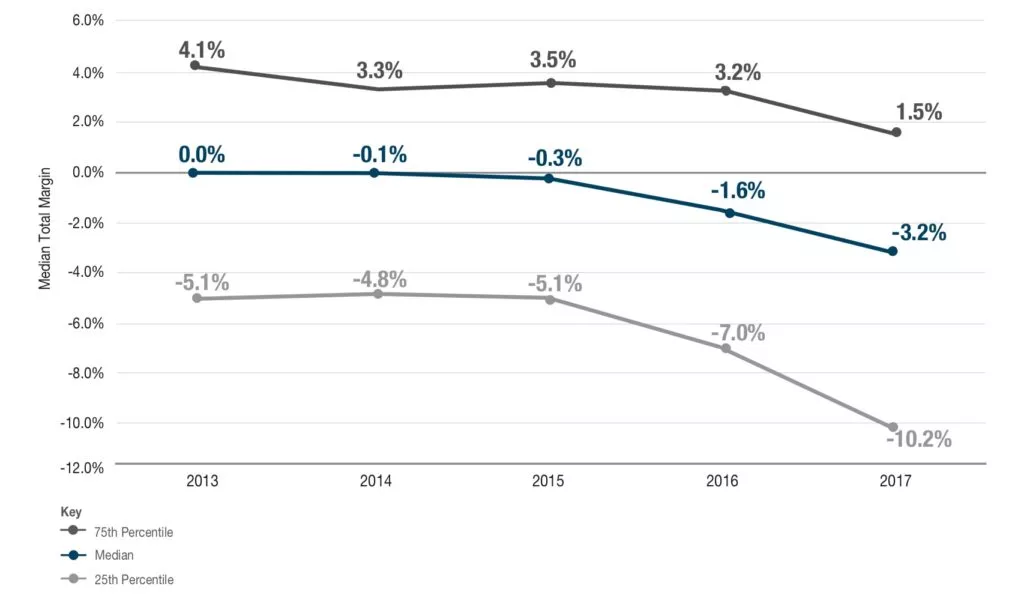
Those shifts had a significant effect on the financial health of the state’s nursing homes, with the overall median operating margin plunging from 0 in 2013 to -3.2% in 2017, the most recent year for which data was available. For the worst performers, those in the 25th percentile of facilities, that figure fell all the way from -5.1% earlier in the decade to -10.2% in 2017.
That overall median number is far below the -0.1% national figure reported by CLA for 2018, a negative margin that the consulting firm described as “an alarming metric” in its annual nursing home cost report, released earlier this year.
It is in line, however, with a Massachusetts-specific report from CLA that pegged the 2017 median margin at -4.1%, rising slightly to -3.5% last year. Based on those numbers, CLA and the Massachusetts Senior Care Association warned that 95 of the state’s nursing homes — about a quarter of the total — were at risk of closure, a bleak projection in a state that has already seen 20 properties shut down over the last year-plus.
“A majority of the Commonwealth’s nursing facilities are operating in the red, particularly those facilities that have a high reliance on state Medicaid funding,” Massachusetts Senior Care Association president Tara Gregorio said in a statement issued earlier this month. “The CLA report clearly shows the situation is dire and the causes are clear.”
Much of the attention has been focused on the state’s Medicaid program, known as MassHealth, with lawmakers passing a $50 million boost to nursing home funding this year. Still, operators assert that the cash infusion isn’t enough, and a consortium of advocates has collected enough signatures to put a major Medicaid funding overhaul on the state ballot next November.
However, Medicaid wasn’t the only reason behind CHIA’s findings. In fact, on an overall basis, Medicare revenue fell the farthest between 2013 and 2017, dropping at a rate of 11.4%; Medicaid revenue, by contrast, only dipped 2.9%.
On a per-resident day basis, revenue actually increased by 10.1% for Medicare, 5.5% for Medicaid, and 7.4% for self-pay residents — but at the same time, expenses saw a median increase of 4.0% over that span, with an overall median revenue increase of only 1.6%, according to CHIA.
“CHIA will continue to monitor this important component of the health care system as the nursing facility industry continues to evolve to meet the changing needs of the residents of the Commonwealth,” the organization concluded.


