Across the U.S., Medicaid rates tend to fall short of the cost of nursing home care for beneficiaries. In the state of Massachusetts, the financial pressures have rendered many skilled nursing facilities unstable — and forced many of them to close.
The trend has also forced many of them to leave bills unpaid, which spreads the pain outside the SNF to vendors and others. For Tara Gregorio of the Massachusetts Senior Care Association (MSCA), it’s a warning sign about the need to stabilize the nursing facility system in the Bay State by fixing its Medicaid problems.
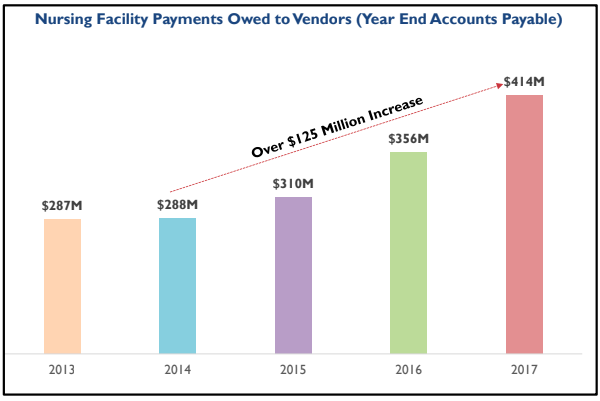
Specifically, nursing facility payments owed to vendors have increased by more than $125 million from 2014 to 2017, with year-end accounts payable rising from $288 million in 2014 to $414 million in 2017, according to a presentation from the MSCA.
“We are grateful that our vendors have a high tolerance and threshold for accounts payable, but when we start to see or hear that vendors are cutting off providers, that’s when we likely will see additional closures,” Gregorio told Skilled Nursing News.
The MSCA is the Massachusetts arm of the American Health Care Association, a trade group for for-profit nursing homes.
The pressures stemming from low Medicaid payments have rippled across the skilled nursing industry in the Bay State. Last year 20 nursing facilities there closed, the highest number of such closures in the past two decades, Gregorio told CommonWealth Magazine in a podcast interview.
The state’s low Medicaid rates under Massachusetts’ Medicaid program, called MassHealth, are a major reason, Gregorio told SNN. It’s a point the organization has stressed before; one deep dive from the Worcester Telegram and Gazette noted, citing data from the MSCA, that accepting more MassHealth patients mean lower profit margins.
“The reimbursement system does not accurately capture the cost of caring for people with multiple diseases, as well as being entirely dependent on assistance with activities of daily living,” Gregorio told SNN.
SNFs in several other states have struggled with low Medicaid reimbursement rates and the pressure it places on their business model. In South Dakota, advocates predicted “statewide disaster” without a boost in Medicaid funding, while other providers in the state of Washington are leaving the space altogether because of the low Medicaid reimbursement. In Wisconsin, nursing homes have blamed Medicaid rates at least in part for closures and financial struggles. Nursing homes in Montana last year sued the state over Medicaid cuts, and when non-profits in Texas shuttered in 2018, they pointed to their state’s low Medicaid reimbursement.
Sen. Ron Wyden, an Oregon Democrat, sounded the alarm most recently on possible cuts to Medicaid during a hearing on safety standards in U.S. SNFs that was held on Wednesday.
“We’ll see proposed another draconian cutback on Medicaid,” Wyden said in his opening remarks. “Medicaid helps cover costs for two out of three seniors in nursing homes. I’m going to fight this proposal with everything I’ve got, because it would turn back the clock on efforts to improve care and it would inevitably lead to more nursing homes closing their doors, which would especially work a hardship in rural America.”
MassHealth bases reimbursement rates on costs from 2007, Gregorio said, and one of the greatest changes since that time period is the higher cost of labor. The low Medicaid reimbursement makes it hard for providers to compete for staff, since the rates don’t match the cost of the workforce. That’s highlighted by 75 cents of every nursing facility dollar being spent on staff wages and benefits, as well as the fact that there are 4,400 direct care nursing staff vacancies as of 2018, according to the MSCA.
To try to address the issue, MSCA is working with vendors to lobby state legislators on the need to support the industry. The MSCA is calling on legislators to invest in the industry in different pieces of legislation and through the budget process, and if both those steps come to fruition, SNFs in the state would see an increase in funding of $75 million. While that would help significantly in stabilizing the sector, the industry is still underfunded by MassHealth to the tune of $350 million each year, Gregorio said.
That comes on top of accountable care organizations (ACOs) that are aggressively managing Medicare beneficiaries, with SNFs in the state seeing a decline of $330 million in Medicare revenue since the passage of the Affordable Care Act in 2010, Gregorio noted.
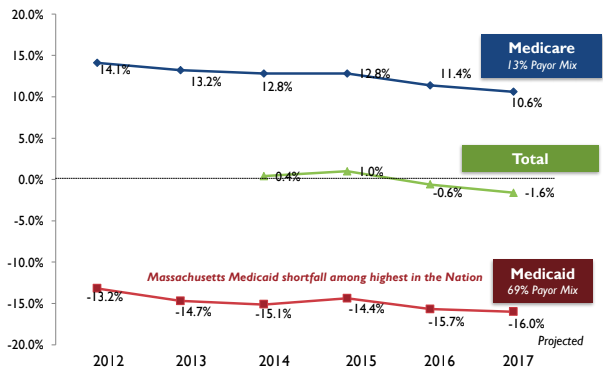
Report: Medicaid Certified Nursing Facilities in Massachusetts: An Analysis of Margins (Oct. 2016, April 2017, Aug. 2017, Sept. 2018). From the MSCA presentation.
The other challenge lies in the changing needs of the patient population, which requires greater investment in staff than years past. Specifically, the opioid crisis has resulted in an increase in younger populations with side effects from substance use disorders over the past two to three years. And hospital partners are increasingly asking that SNFs take care of this population, Gregorio said.
“We are, as a result of the opioid epidemic, seeing more patients, residents accessing our care with immense behavioral health needs,” she told SNN. “And that comes with specialized training costs and staff to ensure that we are providing the best care — as well as safety — for all our residents.”
Companies featured in this article:
CommonWealth Magazine, Massachusetts Senior Care Association



