Private health insurance policies that renew their skilled nursing benefits weekly are more effective in getting patients to reach their rehabilitation goals, compared with Medicare benefits, according to a small study published in the Annals of Long-Term Care.
Samson Barasa of Peace Health Sacred Medical Center in Eugene, Ore., and Donald Jurivich of the University of North Dakota examined the medical records of 234 patients from three large metropolitan nursing homes in Cook County, Ill., for the main insurers for short-term rehabilitation: Medicare, the county-specific Medicaid program County Care, and commercial insurance.
The different patient groups were assessed for how well they reached their physical therapy (PT) rehab goals, with Medicare patient data used as a baseline.
Medicare pays the full cost of SNF care for the first 20 days and requires copayment in the next 80 days, while County Care covers SNF care for 30 days as a bundled package to eligible Cook County residents. Commercial insurance policies renew SNF care support each week if a patient shows progress in reaching his or her goals, the study observed.
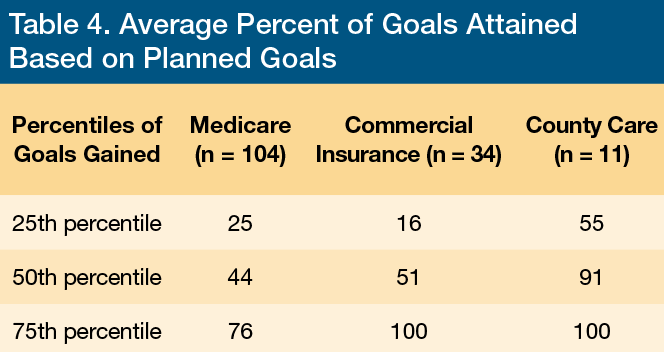
The patients whose skilled care expenses were covered by County Care and commercial insurance had the highest average percent of rehabilitation goals gained at the 50th and 75th percentiles, compared with Medicare recipients, the researchers found. The chances of commercially insured patients achieving more than 40%, 60% and 80% of PT goals was better than those of Medicare recipients, but more modest than those of County Care enrollees.
“Commercially insured patients may do better than patients with other insurance coverage due to a ‘sword of Damocles’ factor — namely, the week-to-week renewal of SNF insurance coverage based on attainment of SNF goals may be a potent factor that drives commercially insured patients toward their rehabilitation goals,” the authors wrote.
PT teams also “favor” commercially insured patients and demand more of them due to the possibility of insurance coverage ending prematurely, the researchers also said. But it’s unclear whether weekly reevaluation of SNF insurance coverage in the absence of progress would be useful for older patients due to a variety of factors, including health.
Written by Maggie Flynn